Forewords
Dr Steve Gardner
CEO PrecisionLife, Chair of Data, AI and Genomics Committee (DAGAC), BIA
The UK has an opportunity to lead the data-enabled health revolution with HDRS, but only if it marries investment in its data ecosystem to intentional and coordinated policy changes that support UK businesses, to enable responsible innovation and create value alongside the NHS.
The coming decade will bring new challenges and opportunities for the UK health and life sciences, including the affordability of healthcare, ubiquitous applications of AI, integration of electronic health and other care records, multiomics, and a clinical system in transition from hospital to home, from treatment to prevention, and from one-size-fits-all clinical pathways to more personalised care.
This report outlines a “North Star” vision for 2035 and sets out a pathway for the future of how health data will be aggregated and analysed to enable UK-led innovative solutions that create value for the NHS and its patients, building a more efficient and effective healthcare system, and ensuring the UK maintains its leadership position in the increasingly global precision and preventive medicine community, supported by its researchers, innovative SMEs, and biopharma companies.
Dr Emma Lawrence
Head of Data Tech Policy and Public Affairs, BIA
In a world where technology is causing unprecedented change, the one constant is data. Data has now become so central to our lives that it is collected, stored, and used throughout our day, without a second thought.
Yet in one of the most important areas of our lives – our health – data is siloed, unstandardised and untapped. Data that could be used to fuel innovation and improve health outcomes remains hard to access and use, a dormant strategic national asset.
This report sets out our vision for a future where improved access to multimodal health data through HDRS is used to transform life sciences. From discovery science, through to clinical trials and clinical care, data will be harnessed to foster innovation to change lives. Health data will ensure that the right treatments reach the right patient at the right time, shifting the move to prevention, precision and personalised care. Importantly, getting HDRS set up from the start to support innovative UK companies will shape better health for NHS patients for years to come, and in tandem drive economic growth and job creation across the country.
Call to action
The decisions made today and over the next five years will determine whether the UK successfully harnesses its health and life sciences data to benefit the population and economy or falls behind the rapidly accelerating global competition. Success will require coordinated policy and action across government, the NHS, regulators, academia, and industry to enable innovation and its adoption.
This should be supported by a mandate on HDRS to prioritise UK value creation with health innovators and job creators, free from short-term revenue targets and enabled by freedom for its leadership to deliver.
Our vision for 2035
Using health data to drive UK innovation
This report sets out a clear “north star” for the UK’s health data ecosystem in 2035. It outlines emerging global trends, the technical and policy capabilities required, and the outcomes the UK should deliver for both its population and its economy.
The UK’s health data is a strategic national asset that has the potential to enable innovations that improve the health of the nation, support NHS sustainability, deliver economic growth and job creation, and drive global life science competitiveness. HDRS and other health data custodians have a critical role to play in using secure access to health data to transform the NHS from a cost centre to a growth engine.
By 2035, the UK's health data ecosystem should function as a unified, intelligent platform powering both a more personalised, preventive medicine healthcare system, and cutting-edge life sciences innovation. Our ambitions for this national resource are to:
- Act as a world-leading exemplar of a secure, ethical, health data research environment that is trusted by clinicians, patients, researchers and the public.
- Use health data to deliver improved population health, sustained economic growth and job creation, supporting a thriving UK life sciences sector.
- Transform the NHS into a research-enabled health system that rapidly evaluates, validates, and adopts data-driven innovations, improving productivity, sustainability and patient care.
- Embed health data across the health system to improve prevention, diagnosis and treatment, delivering better outcomes for patients across the UK.
- Harness health data to accelerate UK-based discovery, development and commercialisation of innovative life sciences products.
- Position the UK as a global leader in data-driven life sciences and AI-enabled biomedical innovation, ensuring the UK remains one of the world’s leading life sciences clusters.
In summary, our vision is clear. When the UK builds a trusted, interoperable, and accessible health data ecosystem, harnesses it for UK-based innovation and commercialisation, and adopts the innovations this enables, it will have created a strategic national asset that simultaneously improves care, strengthens NHS sustainability, improves productivity, and grows a globally competitive life sciences economy, improving both the health and wealth of the nation.
Achieving these goals and capturing their benefits will require policy alignment to support UK-based innovation, clinical trials, and regulation. It will mean using data securely, transparently and ethically, alongside sustained public engagement and a clear demonstration of the benefits that responsible use can deliver to the NHS, its patients, and the UK economy.
To realise the benefits outlined in this vision, HDRS and other data custodians must be positioned as the UK’s strategic gateway for health data. To fulfil this role, HDRS requires:
- A clear mandate to prioritise UK value creation (e.g. UK-based company and job creation) alongside research excellence.
- Freedom to deliver in its governance structure, with aligned support across government departments and regulatory bodies.
Introduction
A pivotal moment for UK health and life sciences data
The UK health and life sciences sector stands at a pivotal moment that demands not just a new gateway to NHS data, but also a deliberate strategy to harness health data as a core national asset to improve health and economic growth. In 2025, the Prime Minister announced the creation of a new Health Data Research Service (HDRS) as a secure, streamlined gateway to UK health and care data to enable innovation and economic growth.
These data, convened through HDRS, are, and will be, a strategic national asset that have the potential to shape the health of the nation, support the long-term sustainability of public services, and drive UK-led innovation, growth and competitiveness in a global economy increasingly driven by AI, genomics, and preventive healthcare. This is not just about creating access to data, but about enabling, validating, and adopting innovation at scale across the NHS and wider ecosystem.
The current model of reactive healthcare is under severe and persistent pressure. Demand for NHS services is rising due to an ageing population, growing prevalence of chronic diseases, improved clinical techniques and medicines, and increasing complexity of care needs. These challenges cannot be solved through NHS capacity expansion alone. To remain sustainable, the NHS intends to shift towards predictive, preventive, and personalised care, intervening before a disease has become untreatable, diagnosing faster, more precisely, and targeting treatment more effectively. This shift will require better data, more sophisticated tools across the care pathway, and, above all, innovation.
Today’s context: demands on health systems
The need for new healthcare solutions is essential and pressing. Global health systems, including the NHS, are recognising that the traditional model of care – treating people once they’ve become sick enough to seek a doctor – is no longer appropriate. Demand exceeds capacity in many parts of the system, and this gap cannot be closed through capacity expansion alone. This is true in most major and developing economies across the world.
Several long-term trends make this challenge more pressing:
- An ageing population, with more people living longer
- The rising burden of chronic diseases, such as diabetes, dementia, cancer, and cardiovascular, musculoskeletal and respiratory diseases
- Increasing multimorbidity, where patients present with multiple complex conditions
- Ongoing workforce constraints and staff shortages, particularly in frontline services
- Escalating economic costs, with healthcare spend rising faster than GDP.
The rising cost of healthcare: People are living longer, but with a much higher burden of major illnesses. Healthcare now costs $10 trillion globally, and over $5 trillion in the US alone (18% of GDP in 2024). These costs are growing at a long-term average of ~1.5% p.a. faster than GDP. Healthcare costs are expected to reach over 20% of GDP in the US by 20336. In the UK, without reform, public health spending is set to rise from 7.9% of GDP in 2024/25 to 14.5% by 2073/74. This means that the UK will be spending £1 for every £7 of its national wealth on healthcare.
In England alone, over 14 million people have multiple long-term health conditions. These diseases are progressive and expensive to manage. As a result, they consume around 70-80% of healthcare spending, and lead to significant additional burdens in social care and lost economic productivity. Without change, the economic impact and social cost of avoidable disease will continue to rise sharply as the population ages.
Yet these outcomes are not inevitable. Many chronic diseases can be prevented or delayed if detected early and managed effectively. This requires:
- Earlier identification of risk before symptoms manifest
- Better diagnostic tools to catch disease at a treatable stage
- Personalised interventions tailored to individual need and delivered at the right time.
This is the core logic of a transition to predictive, preventive and personalised care, with data and innovative tools as the enabling foundation. High-quality, linked health data and aligned policy changes will be fundamental to this change.
A transformation in health and life sciences
In parallel, life sciences innovation is undergoing a fundamental transformation that is enabling predictive, preventive and personalised care. Increased computing power and modern data science mean large datasets can drive new discoveries. AI-enabled research, multi-modal diagnostics, and data-driven drug discovery are changing how new medicines and technologies are developed, validated, and adopted.
2035: global competition is accelerating
Countries around the world are investing heavily in national initiatives to connect clinical data with research datasets, including genomics, imaging, and real-world outcomes.
The UK has world-leading foundations, including a strong life sciences research base, innovative and entrepreneurial SMEs, internationally respected regulators, and a health system with potential to generate real-world, population-scale evidence. However, global competition is accelerating, and the UK will be left behind without deliberate action. Sustaining that leadership to 2035, and fully capturing its health and economic benefits, requires deliberate, coordinated action now.
The UK is widely recognised as a global leader in life sciences, underpinned by an unparalleled convergence of health and genomic data, clinical research, and innovation capability. However, the international landscape is shifting rapidly. Countries are investing at scale in sovereign data infrastructure, national genomics programmes, and AI-driven healthcare systems.
The UK is not the only choice for health data and competition will be even greater in 2035 - there are already over 200 large scale patient datasets globally, connecting primary and secondary healthcare data with genomic information. Several national projects target cohort sizes in the 100k–multi‑million range, and have already developed large scale genomics repositories.
The global landscape
Large-scale, integrated clinical and genomic datasets are now an established global standard for research-ready health data infrastructure. Examples include Our Future Health, All of Us, FinnGen, and other national programmes in China, EU, Russia, Qatar, Saudi Arabia, Iceland, Singapore, Australia, and the UAE.
Large US health systems such as Kaiser Permanente Research Bank, the Veteran Association’s Million Veteran Program, Geisinger, Mass General Brigham, and Truveta are running similar projects with the explicit aim of using the resources to lower the cost of care and improve patient outcomes.
By 2035, the UK will be operating within a dynamic and competitive global data landscape shaped by technological, economic, ethical and geopolitical factors. While some will be smaller in population than the UK, they are big enough to facilitate most research projects. The differentiators that commercial users will look for in choosing datasets to access will no longer be size alone but will include:
- Predictability and speed of access
- High quality multiomic data with up-to-date integration of longitudinal care records and outcomes
- Ability to recontact consented patients and enrol them efficiently in clinical research
- Regulatory clarity and innovation-enabling policy and contracting
- Clear and fair benefit-sharing mechanisms.
Health data is increasingly being treated as a sovereign national asset closely linked to long-term national security, resilience and economic advantage. Many countries are strengthening domestic oversight of how their health data is stored, accessed, and used, including measures that constrain cross-border data flows.
HDRS has the potential to act as a catalyst for this transformation, accelerating innovation, adoption, and value creation across the health and life sciences system.
A strategic opportunity for the UK
The changing dynamics in health and life sciences represent a significant opportunity for the UK, but others have recognised this as well. Health data is not a by-product – it is one of the strategic foundations for better care, stronger research, and a more competitive economy driven by life sciences innovation. This is the Government’s ambition for HDRS, but the UK must act with purpose and boldness now to secure the future of its healthcare system and its global leadership in life sciences.
The opportunity
Health data as a national growth engine
The UK has already invested in building a world-leading health data infrastructure, genomic capabilities, and NHS operational know-how. Together, these constitute a strategic national asset with significant economic and societal potential. Without deliberate policy intervention, the UK risks continuing a pattern of creating high-value, world-leading clinical and scientific capabilities, while letting much of the downstream economic value be captured elsewhere. This would result in the NHS re-importing these products at market prices, while the UK fails to benefit from the job and economic value created through UK-based innovation and commercialisation.
Proper protection and use of healthcare data can increase GDP by creating new export sectors, high-value jobs, inward investment, and a positive fiscal multiplier from existing assets. It can also improve public sector productivity from NHS efficiency gains, lower the cost of care delivery, and reduce the number of people who are long-term out of work.
By encouraging and supporting innovators to grow and deploy in the UK, we can tackle both the health and economic challenges. It is therefore critical that the UK invests in its data ecosystem and opens it up to support a vibrant community of UK-based businesses that can develop innovations responsibly and create value alongside the NHS.
AI solutions will become a critical backbone of all NHS services in the next decade. It would be a devastating blow economically and for national security if this market was monopolised by large foreign businesses, able to sell solutions to the NHS built on UK patients’ data because they were better resourced to access data and bring products to market.
The risk is already emerging. Almost all of the data storage, compute and AI platforms used by researchers and the NHS today, i.e., data centres, cloud computing, federated health data platforms, electronic health record (EHR) systems, trusted research and secure data environments, AI frameworks, large language models, etc. are owned by offshore organisations. The potential for impacts on data and service accessibility, data privacy and public trust, economic growth, and even national security, should be considered carefully when choosing infrastructure providers and negotiating contractual terms around data.
A soft power of opportunity
By 2035, the UK’s integrated data infrastructure will not only support a more efficient and effective domestic health system but also position the UK as a trusted and collaborative global partner in health data – grounded in strong ethical foundations and recognised for innovation leadership. In a world increasingly shaped by how data is governed, shared, and used, the UK has an opportunity to lead ethically, competitively, and in partnership with others.
Innovation for value creation
The value created by innovations from UK SMEs that can prevent ill-health and improve clinical efficiency could significantly outstrip the revenues that could be created by subscription fees.
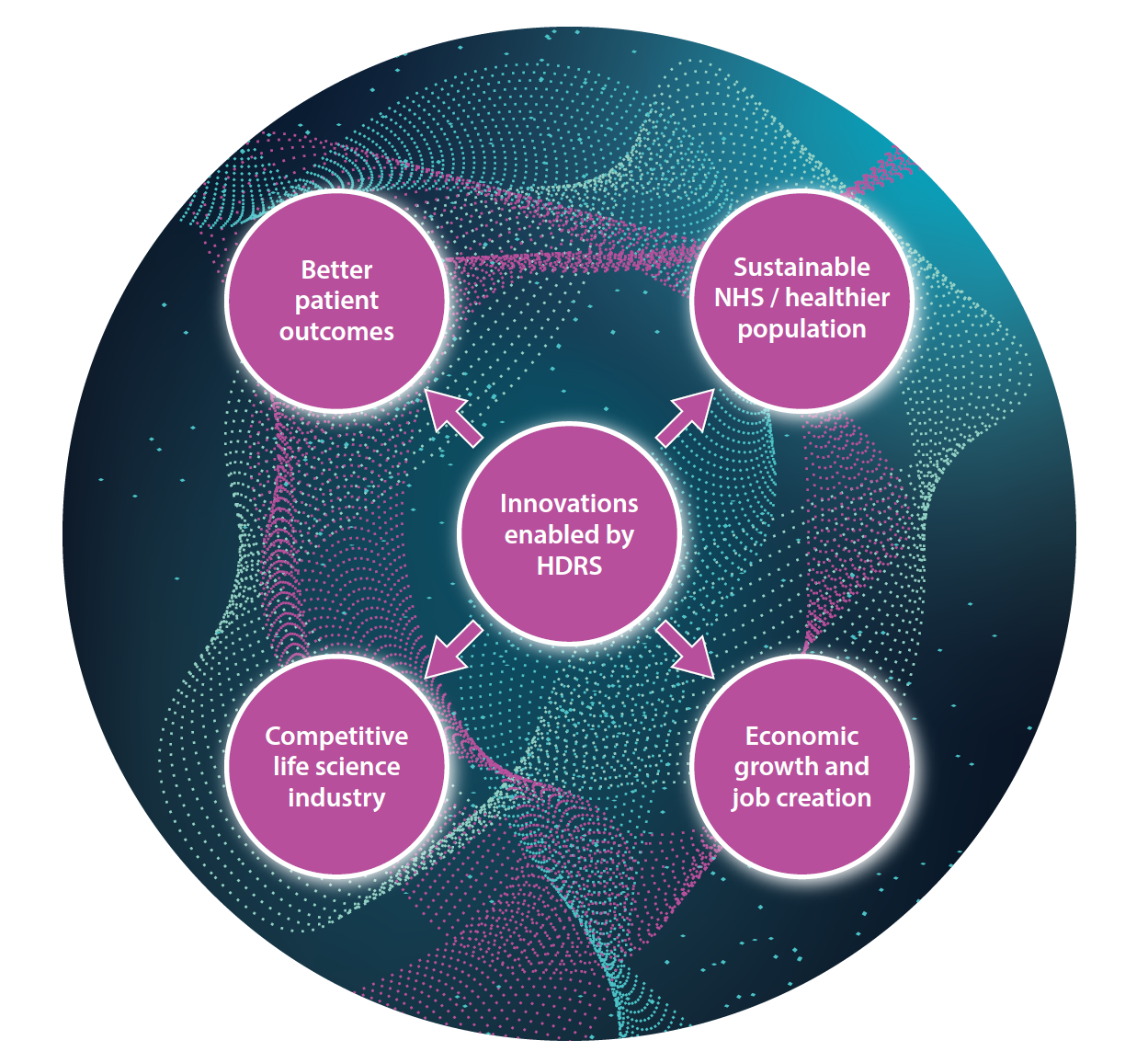
Innovations enabled by health data have the potential to create value across four interconnected domains, each with overlapping but distinct requirements and benefits:
Value to patients
- Earlier detection and faster diagnosis, reducing time to treatment and avoidable deterioration
- More personalised treatments, improving efficacy and reducing side effects
- Better long-term outcomes and quality of life through convenient, proactive monitoring and timely adjustment of care
- More convenient, less fragmented care through digital health apps, remote monitoring, and fewer unnecessary appointments
- Smoother transitions across care settings as data follows the patient across pathways
- More holistic, joined-up care, enabled by integrated data that gives healthcare professionals a complete view of a patient’s history, needs, and outcomes across the care pathway
Value to the NHS
- Fewer avoidable admissions and late-stage presentations through earlier intervention
- Reduced duplication of tests and appointments through shared longitudinal records
- Safer prescribing and fewer adverse events through better risk prediction / monitoring
- Improved operational planning and service productivity through AI-enabled optimisation
- Better targeting of resources to high-need populations and prevention priorities
- Faster learning about what works, for whom, and why – supporting pathway redesign based on real-world outcomes
- A better workforce experience for health professionals, giving time back to patient facing interactions and ensuring they can deliver the highest quality care.
- Collaboration and knowledge exchange, embedding clinical and commercial two-way learning- ensuring the NHS benefits from solutions it needs and health professionals can actively contribute to research and innovation
Value to life sciences research and innovation
- Clearer understanding of disease biology and progression across diverse populations
- Development of new devices/technologies for disease detection, diagnosis and treatment beyond medicines (e.g. in radiology, pathology and robotics)
- Discovery of new drug targets, biomarkers, and repurposing opportunities
- Faster identification of cohorts and more representative recruitment into trials
- More efficient clinical trial follow-up using routine outcomes and patient-reported measures (PROMs)
- Stronger safety monitoring and real-world effectiveness evidence after deployment (of both medicines and devices)
- AI-driven innovation across the pipeline, from target identification and validation to trial design and post-market surveillance
Value to the UK economy
- Improved sustainability of the NHS and social care, higher economic productivity and increased job creation
- A healthier UK population, driving wider economic benefits across overall UK productivity
- Increased inward investment and global partnerships anchored in UK capabilities
- A pathway for UK SMEs to scale from discovery into clinical adoption and export
- Higher R&D productivity and faster translation of innovation into real-world impact
- Global leadership in AI, diagnostics, precision medicine, and data-enabled clinical trials
How health data will transform life sciences innovation
Health data will also transform how life sciences innovation creates value, particularly in biopharma research and development.
The trend away from a ‘one-size fits all’ care pathway to more personalised treatments is well-established in oncology. By 2035, the integration of high-quality health and life sciences data with AI tools will drive this further across more complex chronic diseases. However, for us to be able to develop medicines for smaller patient groups means we will need to find more efficient ways to develop and deliver those medicines, or they will be unaffordable.
Call out box: Types of AI and their applications
Artificial Intelligence (AI) is used as a shorthand for a wide variety of technologies that learn patterns from data to make decisions, predictions, or generate new responses. "AI" is not however a single technology but a toolkit of approaches with different strengths, and potentials for bias and error. Familiar tools like ChatGPT or Perplexity represent only one category within a much broader field.
Some AI systems such as Convolutional Neural Networks (CNNs) are deterministic: given the same input, they will always produce the same output. Others are probabilistic and can produce variable responses even to identical prompts. This distinction has significant regulatory and safety implications. In medical imaging (e.g., detecting signs of cancer), consistency and auditability are essential. CNNs will produce the same result each time from the same image, making it possible to test, validate, and regulate to high clinical standards. Large Language Models (like ChatGPT), by contrast, are trained on vast, often uncurated text datasets, enabling them to generate plausible responses with remarkable flexibility but limited transparency. They are known to hallucinate (invent non-factual responses), and give different responses if there are small variations in inputs or training. This introduces new challenges for assurance, accountability, and compliance, particularly within safety‑critical and regulated environments.
Understanding these differences is essential for effective technology selection, policy design, public communication, and governance frameworks that enable innovation while maintaining trust and safety.
New discovery projects will increasingly focus on targeted precision medicines. Patient stratification biomarkers will become crucial to identify different drivers of disease and predict which drugs to use at what doses for individual patients so that they are more effective, safe, and tolerable.
Use of health and genomic data has already significantly de-risked pharmaceutical R&D. By 2035, advances in multi-modal AI powered by large-scale, AI ready datasets will enable:
- Better target and causal biology discovery, moving beyond traditional genome wide association type studies (GWAS) signals to find and validate more functional, actionable targets and mechanisms, predict molecular structure and interactions, and systematically identify druggable genes associated with disease resilience.
- Precision medicine for common conditions, with patient stratification biomarkers enabling more effective treatments with improved safety and tolerability, including new precision approaches to complex conditions such as diabetes, cardiovascular disease, respiratory illness, and dementia.
- Improved cohort stratification by mechanism, enabling smarter trial design and higher clinical success rates.
- AI-enhanced diagnostics, decision support and trial delivery, delivering better regulatory strategies, trials designs, and opportunities for new complementary diagnostic/prognostic tools based on genetic, imaging, pathology, dermatology, and biomarker tests.
- Accelerated drug discovery and development, supported by high-performance compute (GPUs/TPUs and quantum) and semi-virtualised “lab-in-the-loop” automation
- Faster development of targeted therapies, including new modalities such as AI-driven antibody discovery, therapeutic mRNA vaccines, and antisense oligonucleotides (ASOs)
Clinical trials and regulatory
These drivers have the potential to unlock new, more targeted medicines for patients, but data and innovations alone are not enough. For the UK to be a competitive site for future biomedical research, it will be essential for the NIHR, MHRA, NICE, and the NHS to share data and work together effectively to accelerate their validation and adoption. This will enable accelerated clinical trials approval, feasibility and recruitment, and the rapid market entry, adoption, and reimbursement of stratified precision and preventive treatments.
Smarter clinical trials help capture value for new innovations by providing a path to rapid approval and adoption. Patients will need to be consented for commercial research and available for recontacting to participate in trials and long-term evaluation of outcomes, building on capabilities developed through NHS Digitrials.
Trial recruitment will often start outside the healthcare environment. Speed and flexibility of trial design and the ability to recruit patients efficiently and cost-effectively based on specific genetic/multiomic/clinical biomarkers will become paramount to global competitiveness. As a research consented cohort, Our Future Health already operates its Clinical Research Recruitment Service to facilitate that type of genotype/phenotype targeted trial-based recontacting, with high recruitment rates, and this model should be extended.
By 2035, patient reported outcome measures (PROMs) will be used more frequently and many lower-risk trials and post-marketing surveillance will be delivered remotely using wearables (activity, heart rate, ECG, sleep etc.) and PROM surveys via apps. Collecting more reliable real-world outcome data will enable payments to be based on value to the health system and patients, decreasing the incentive to push for increased prescription volumes for drugs that are not widely efficacious or tolerable for patients. The same tools can also be used to refine clinical care pathways, ensuring that effective treatments reach the right patients more quickly.
Real-world impact: evidence of UK innovation
New innovations based on the use of large-scale patient data have the potential to deliver billions of pounds of benefit per year to the NHS and its patients.
(Brainomix) Stroke – estimated AI-assisted stroke imaging was highly cost-effective, generating >£40 million in cost savings and >1,000 additional QALYs per year in England.
(PrecisionLife) Diabetes– an AI prognostic test that can accurately identify type-II diabetes patients who have a high risk of renal failure early enough to intervene and reduce the need for dialysis by 30%. If adopted for all newly diagnosed diabetics across the NHS, after accounting for all costs (and commercial profits), this single test could save the NHS over £2 billion in the coming decade and create a new global scale UK diagnostics company.
(Mendelian) Rare diseases – MendelScan uses AI-driven pattern mapping of electronic health records to identify patients at risk of rare diseases before clinical suspicion. Early identification of DiGeorge syndrome alone is projected to save the NHS ~£476,000 over five years, with ongoing annual savings of ~£150,000. Scaling this approach across multiple rare diseases could generate substantial additional savings, while improving patient experience and outcomes.
(Jiva.ai & Aevice Health) Asthma – AI-enabled remote patient monitoring using continuous respiratory data is being developed to predict asthma exacerbations and provide early warning of deterioration, enabling earlier intervention and proactive disease management. Preventing just 10% of asthma-related hospital admissions, over 60,000 annually in England, could save the NHS £50–£70 million per year, alongside substantial reductions in avoidable morbidity and improved patient outcomes.
(CardiaTec Bio) Cardiovascular Disease – AI-driven target discovery using multimodal human data can significantly increase the success rate of novel cardiovascular therapies by identifying causal disease drivers earlier. Enabling the development of more effective treatments for conditions such as heart failure and atherosclerosis, could reduce hospitalisations and late-stage interventions, which currently cost the NHS billions annually. Even a modest improvement in treatment efficacy and patient stratification could translate into hundreds of millions in savings over a decade, while substantially improving survival and quality of life for patients.
Looking ahead: a 2035 patient journey – data powered, AI enabled personalised care
By 2035, leading global health systems will have implemented transformational changes in the way people access and use healthcare, supporting them to stay healthier for longer. Patients will engage with the health system through AI and data-enabled tools, accessing care services that are more responsive, personalised, and convenient for them.
A patient’s digital record in 2035 will integrate real-time updated longitudinal primary and secondary care history, prescribing and dispensing data, diagnostic data including lab tests, imaging, and pathology, outcomes and patient-reported measures (PROMs) and wearables, genomics and (where appropriate), other omics data. Together, this integrated data record will support a radically improved experience of care. Patients will benefit from:
- Continuous health screening, powered by genomics, electronic health record and wearables data, to predict disease risk, identify early warning signs, and guide tailored prevention strategies and lifestyle advice
- AI-enhanced diagnostics delivering faster, more affordable, and more accurate interpretation of imaging, pathology, and laboratory tests – reducing time to diagnosis and referral, and avoiding unnecessary interventions
- Personalised risk stratification and treatment, using AI and predictive models to tailor care plans to each individual’s genetics, health history, treatment response, and real-time data from wearables or apps
- Virtual and remote care tools, including conversational AI, digital health apps, and digital twins to support home monitoring, triage, self-referral, and behavioural nudges – making care more proactive and accessible
- Seamless transitions between settings, with data flowing securely between primary, secondary, and to support integrated pathways and continuity of care
- Automation of routine clinical and administrative tasks, including note-taking, document processing, appointment scheduling, e-prescription, referral letters, and bed occupancy management – freeing up clinician time and improving quality
- Expanded role of robotics and AI in procedures, enhancing precision, safety, and support in complex or routine interventions
Integrated NHS data should be used to foster innovations in clinical efficiency and precision & preventive medicine. Adopting these in routine clinical practice is a key route to value creation for the NHS and its patients. This has the potential to save tens of billions of pounds in health and social care spending, while improving outcomes for patients and the UK economy.
Taken together, this can convert the NHS from a cost centre into a growth engine, while the cost savings achieved through adoption of homegrown solutions creates sustainable funding. Export revenues offset the investment and can create high-skilled jobs in the UK.
Delivering the vision
Invest for the long term, reap multiple benefits
Delivering this vision will require coordinated action to harness UK health data, convened by HDRS, to support UK-based innovation and commercialisation. By adopting the innovations it enables, we can improve care, strengthen NHS sustainability, improve productivity, and grow a globally competitive life sciences economy.
The next five years represent a critical window to build the infrastructure, public trust, governance frameworks, and delivery capability needed to capture this opportunity.
This will require significant investment, but it has the potential to pay back many times for decades to come. The use of patient data to enable prevention and earlier, more effective interventions across chronic diseases has the potential to transform the efficiency and affordability of the NHS, saving tens of billions of pounds per year and improving the lives of tens of millions of people.
HDRS should be given a clear mandate to help drive UK value creation, through supporting UK-based innovators and job creators, alongside research excellence, ensuring that the benefits of data-driven innovation are realised for UK patients, the NHS, and the wider economy.
HDRS can play a critical role, alongside other health data custodians, in enabling the responsible use of health data for research and innovation. This will unlock significant economic growth, support home-grown innovation, and deliver better outcomes for patients. Done poorly, the UK risks losing its competitive advantage in data-driven life sciences, with consequences for the economy, the NHS, and patient care alike.
Delivering this vision by 2035 depends on HDRS having a clear objective of UK value creation and working in coordination with other data custodians to ensure that UK SMEs and innovators can access the UK's health data without prohibitive cost or complexity. It will need to operate free from short-term revenue targets, with the freedom for its leadership to deliver, and with aligned support across government departments and regulatory bodies. This phase must shift beyond strategies, minimal viable products, and pilots into consistent implementation across the NHS and the wider healthtech and life science ecosystem.
Realising the full value of health and life sciences data will require coordinated action across regulation, funding, procurement, and delivery. Innovation will not scale through technical progress alone: the system will need clear pathways from validation to adoption, incentives that reward outcomes, and operational models that enable safe deployment in real clinical settings. With a coherent, pro-innovation policy and investment landscape, the UK can unlock long-term value for patients, strengthen NHS sustainability, and grow a globally competitive health and life sciences sector.
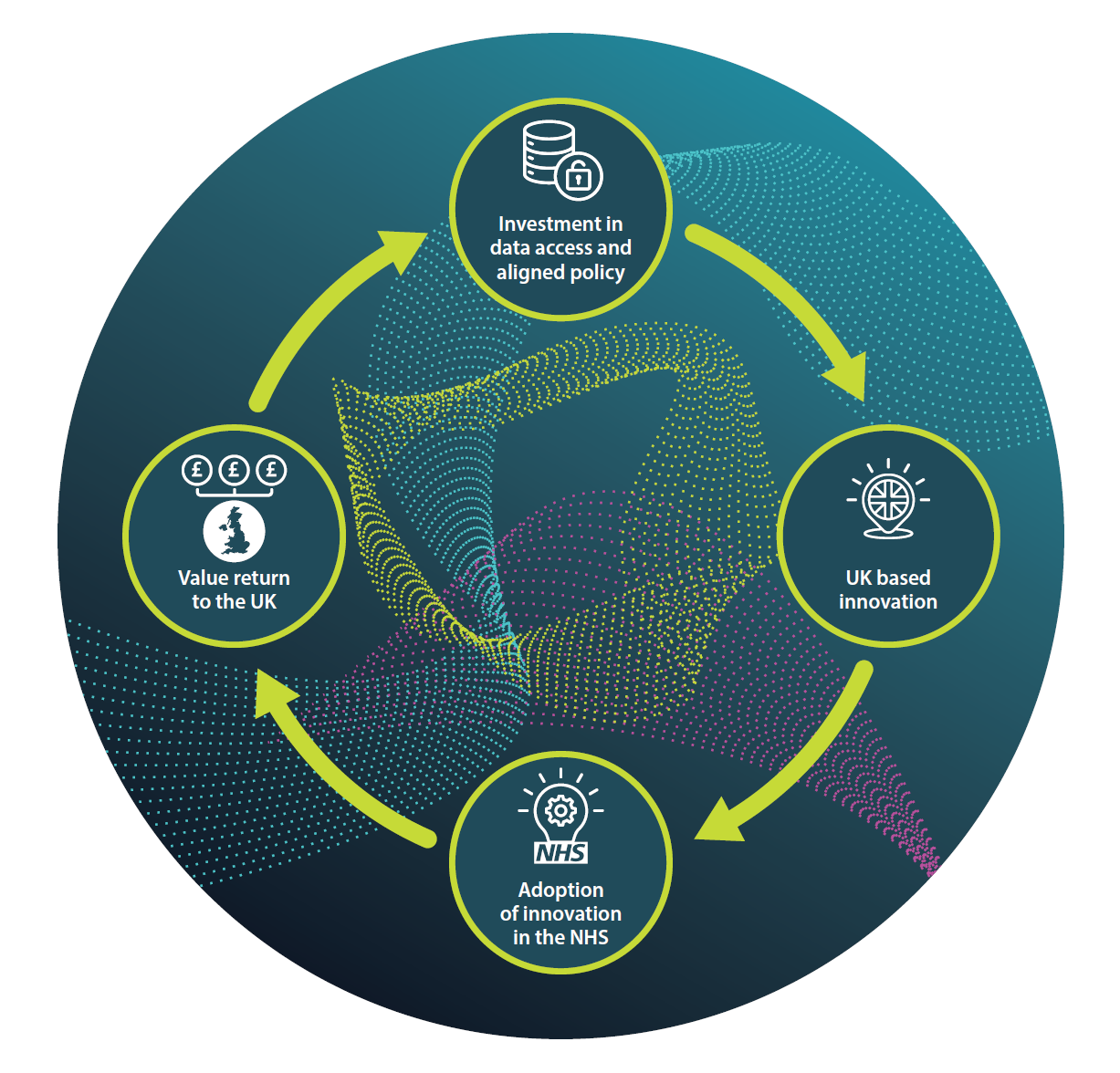
However, realising this value is not automatic. For the UK to harness these opportunities, it needs to develop a health data ecosystem that can power home-grown innovation and adoption, while incentivising value creation in the UK.
Enabling UK SMEs to capture value from health data
Facilitating access to HDRS health data should be a core part of the UK’s industrial strategy. This means aligning data access, funding, and policy to support UK-based innovators and job creators to develop and scale within the UK. This investment will pay dividends in improved health outcomes and economic growth, while increasing our sovereign capabilities.
Previous estimates of NHS data value have misunderstood how value is created, overestimating raw data and underestimating the value-add of downstream innovation. These historic models have assigned far too high a value to a single source of raw data, and too low a value to the impact that innovations derived from data can create.
The world has moved significantly in the last 10 years, and much more detailed data have become widely available at much lower prices. Multiple sub-national sources of genomic plus longitudinal clinical/prescription data are now available to SMEs for £9K-£40K / year.
High pricing restricts access, hindering innovation and reducing long-term value through improved health outcomes, NHS savings and economic growth. This will have a significant impact on the return on investment. As an example, the cost of accessing Our Future Health (OFH), one of the best and largest currently available research datasets with participant recontact capabilities, is £40K-£320K per year with no downstream IP/commercial rights. This annual subscription price (which includes a 50% discount) is significantly inhibiting its uptake, especially among SMEs. Of the 61 data users at 31 Dec 2025, only two UK SMEs accessed OFH datasets – one of which is a development partner of OFH.
There are many things to consider when devising potential pricing models and access terms:
- Companies and shareholders/investors’ opinion on downstream royalties, equity stakes, or other participation in exit valuation without significant co-investment
- Companies and their shareholders/investors will not accept disclosure or risk to of any background IP including their very high-value AI models and analytics platforms
- Pricing subscriptions that are too high (at a point where only major tech companies can access it) will bias access to well-funded foreign companies, effectively disadvantaging and/or excluding more poorly funded UK companies
Lowering the financial bar to data access from HDRS and other custodians will incentivise increased access by SMEs, which will in turn increase the prospects for data-driven innovation leading tobetter health and more value creation for the NHS and its patients (see box Real-world impact: evidence of UK innovation). It will also create value in the UK through economic growth – this outweighs the return that could be generated by subscription or access fees.
HDRS within the UK health data ecosystem
The UK benefits from a rich and diverse landscape of health data custodians, spanning national data banks, NHS-led secure data environments, and large-scale research programmes. Together, these organisations represent a unique and globally significant resource, underpinning advances in research, clinical care, and innovation.
Realising the full value of this ecosystem will depend on enabling secure, timely and efficient access to data across this ecosystem. Within this context, HDRS has the potential to act as a strategic gateway, working alongside existing custodians to enable responsible data use, reduce complexity, and support innovation that improves patient outcomes and drives UK economic growth.
Five pillars of the health data ecosystem
We envision the UK’s health data, convened through HDRS, as a vital national resource that fuels a new era of home-grown innovation. By bridging the gap between data, discovery and adoption, we can transform patient outcomes, secure the long-term future of the NHS, and cement Britain’s status as a global life sciences superpower.
By 2035, the UK’s health data ecosystem should function as a unified, intelligent platform powering both healthcare and cutting-edge life science innovation.
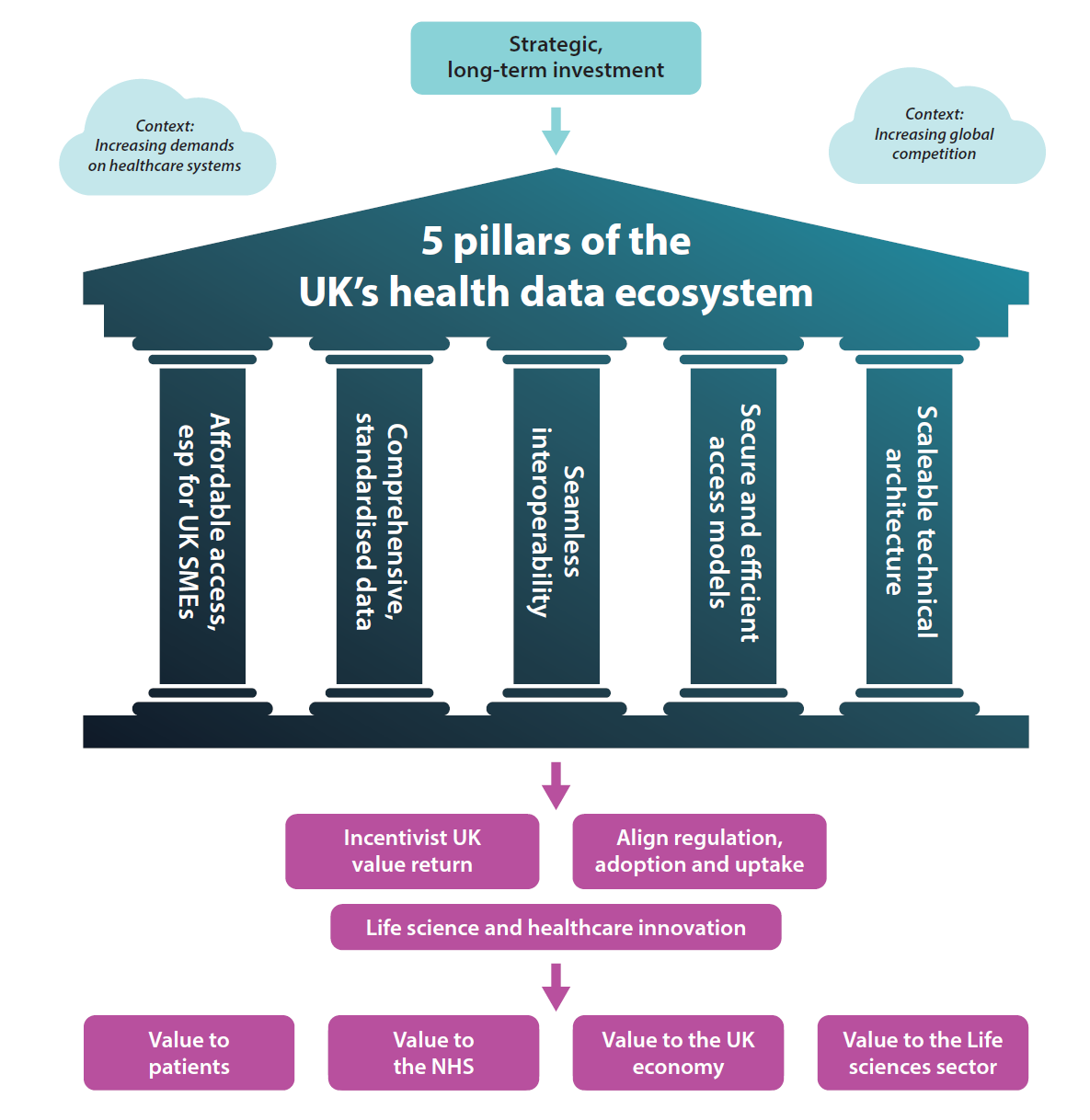
This platform should be built on five interdependent pillars focused on:
- A secure and robust governance and funding framework, including affordable access for UK SMEs, free from competing revenue targets, that ensures secure, legally compliant and ethical use, value return to the UK, and industry co-development.
A governance framework that provides both strong, effective, protection for patients and is enabling for UK-based innovators– designed to support secure data access while delivering benefits and value to the NHS and its patients at pace.
- Collection and standardisation of comprehensive data including genomics: standardised across longitudinal multimodal sources
Large-scale integrated clinical and genomic data, including functional genomics, imaging data, unstructured data, wearables and real-world evidence with data quality standards designed to support equitable representation across diverse populations.
- Seamless integration across systems and data types, with up-to-date records and common standards across all four UK nations, supported by defined interoperability standards governance
Seamless, secure access to diverse, high-quality datasets, alongside governance structures and common data standards.
- Secure and efficient access models that are streamlined and timely, offering different data and access models for different users and applications, underpinned by clear lawful bases for processing and transparent consent and opt-out frameworks
A modern, flexible and high-performance technical architecture capable of handling large-scale, multimodal health data. This infrastructure will support both care delivery and world-leading research, while reflecting the increasing complexity of real-world data environments.
- Resilient, flexible and scalable technical architecture that is capable of enabling AI and other innovative clinical solutions
A resilient, future-proof data system will need to support diverse data access and integration models, analytical methods, high-throughput AI workflows, and collaborative projects across multiple sectors and geographies
A balanced approach to data sovereignty
For the UK, data sovereignty should not mean closing the door to global collaboration. The UK should continue to lead in science through international partnerships, while ensuring that NHS and health data is governed in the public interest, that public trust is protected, and that the value generated from UK health data – whether through improved outcomes, NHS productivity, new jobs, and/or commercial innovation – is captured and returned proportionately to patients and the UK economy.
Conclusion
The UK has a generational opportunity to lead the world in responsible, data-enabled health and life sciences. With the NHS, world-class research, trusted regulation, and a vibrant home-grown innovation ecosystem, the UK has the foundations to build one of the most impactful health data environments globally. However, continued leadership to 2035 is not guaranteed.
By building a trusted, modern, and interoperable health and life sciences data ecosystem, convened through HDRS, the UK can:
- Enable the discovery, approval, and adoption of life-saving innovations, supporting UK SMEs and home-grown innovations
- Create high-skilled jobs and long-term economic growth by enabling UK-based innovation and commercialisation
- Deliver better, faster, more personalised and preventive care for patients
- Strengthen the long-term sustainability of the NHS
- Earn global trust as a steward of ethical and inclusive data use
This future will not happen by chance. It will require coordinated policy and action across government, the NHS, regulators, academia, and industry – supported by sustained investment in infrastructure, workforce skills, and enabling governance, with a clear focus on delivering public benefit and economic growth.
HDRS can play a critical role as a catalyst for this transformation, enabling innovation, adoption, and long-term value creation.
The decisions made in the next five years, and the utility of the resources built will determine whether the UK continues to lead or begins to fall behind, and how successfully we will be able to transform the nation’s health. We invite policymakers, regulators, NHS leaders, researchers, and innovators to align behind this vision and turn ambition into action.
Rccomendations
For Government:
- Give HDRS A clear mandate to prioritise UK value creation (e.g. UK-based company and job creation) alongside research excellence
- Grant HDRS Freedom to deliver in its leadership and governance structure, with aligned support across government departments and regulatory bodies
- Align regulation, funding, procurement, and delivery, through clear pathways from validation to adoption, incentives that reward outcomes, and operational models that enable safe deployment.
For Health data custodians:
- Ensure a secure and robust governance and funding framework is used, including affordable access for UK SMEs, free from competing revenue targets, that ensures secure, legally compliant and ethical use, value return to the UK, and industry co-development
- Focus on the collection and standardisation of comprehensive data including genomics: standardised across longitudinal multimodal sources
- Work towards seamless integration across systems and data types, with up-to-date records and common standards across all four UK nations, supported by defined interoperability standards governance
- Develop secure and efficient access models that are streamlined and timely, offering different data and access models for different users and applications, underpinned by clear lawful bases for processing and transparent consent and opt-out frameworks
- Invest in resilient, flexible and scalable technical architecture that is capable of enabling AI and other innovative clinical solutions
